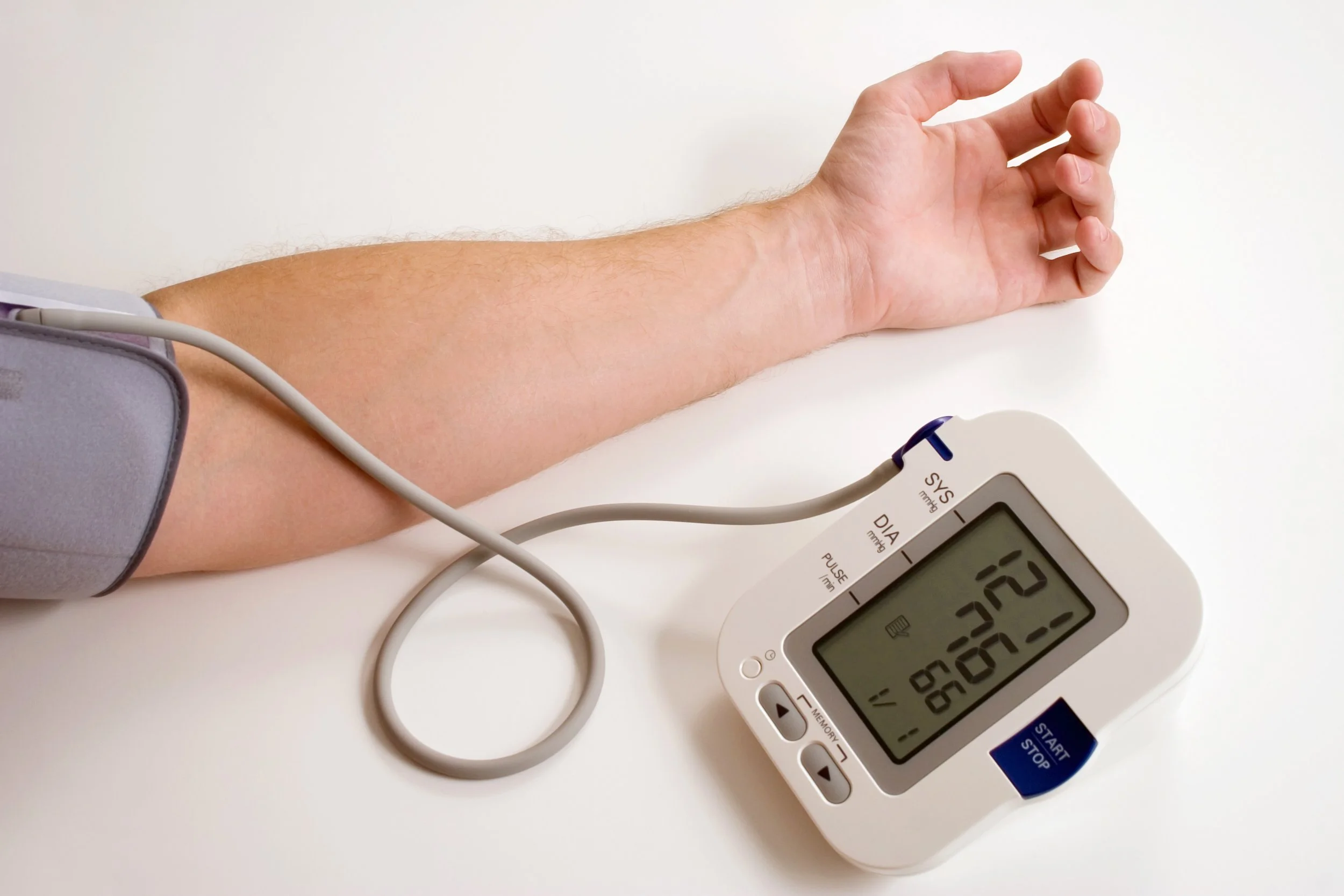
Blood Pressure Monitors Guide
A practical guide to choosing a home blood pressure monitor — with accuracy front and centre.
Last reviewed: April 2026
High blood pressure (also called hypertension) is common as we get older — and it often has no obvious symptoms. That’s why home monitoring can be so valuable: it helps you spot patterns over time and keep a clear record to share with your doctor.
At the same time, buying a monitor can feel surprisingly confusing — especially online, where many devices look similar.
Our goal here is to help you choose a monitor you can trust, understand the features you’ll see on modern devices, and take readings at home in a way that produces consistent, useful results.
If you’re new to the topic, you may first want to read our overview of what high blood pressure is and why it matters.
Important:
This page is for general education and does not replace medical advice. If you’re worried about your blood pressure, speak with your doctor or a qualified healthcare professional.
Why choosing a home monitor can be difficult (and how this guide helps)
Buying a home blood pressure monitor should be simple. In practice, it isn’t — because:
There are huge numbers of devices online, and they don’t all meet the same standards.
Some devices look professional but haven’t been properly tested for accuracy.
For example, a 12‑month analysis across 10 countries published in the Journal of Hypertension reported that around four out of five devices in Amazon’s top 100 best‑selling lists had not passed adequate clinical validation testing. View the study abstract.
(That doesn’t mean every unvalidated device is inaccurate — it means you often can’t tell whether it’s accurate without proper testing.)
Cuff size matters, and the wrong fit can make readings unreliable.
Features can be confusing, and it’s easy to pay for extras you won’t use.
This guide focuses on the things that matter most:
Accuracy (clinical validation)
A cuff that fits properly
A monitor that matches your needs and preferences
If you want to skip the theory and go straight to a shortlist of monitors we consider good options (based on clinical validation and usability), start here:
The most important rule: choose a clinically validated monitor
What “clinically validated” means
A clinically validated monitor has been tested in a formal study comparing its readings with measurements taken by a trained clinician using recognised methods.
In plain terms: clinical validation is how you know a monitor’s readings are likely to be trustworthy.
Clinical validation usually includes:
Use of modern testing protocols
Independent verification of accuracy
Results published in a peer‑reviewed journal
If a device hasn’t been validated, there’s no reliable way to know whether its readings are accurate — even if it has lots of reviews.
What do medical guidelines say? UK and European guidance consistently emphasises the use of clinically validated home monitors.[1, 2, 3, 4]
If you’re going to share home readings with your doctor, using a clinically validated device matters because it increases confidence that your readings reflect your true blood pressure rather than device error. Some research also notes that when validated monitors are used with good technique, home readings can support clinical decision‑making. Read the paper.
Where to check clinical validation
Some organisations maintain public lists of clinically validated devices. [2, 3, 4] These can help you double‑check a model name before you buy:
STRIDE BP (European Society of Hypertension co‑sponsored): validated home devices list and searchable database
British & Irish Hypertension Society (BIHS): patient‑friendly list of trusted monitors
German Hypertension League (Deutsche Hochdruckliga): certified devices list (PDF)
Medaval: device lists and certification (useful for cross‑checking validation evidence)
(These are external sites. Device availability can vary by country, and model names sometimes differ slightly between regions.)
A quick note on monitor age
Even a good monitor won’t last forever. As a rule of thumb, a newer device is more likely to match current standards. If you’ve had a blood pressure monitor for years, it’s worth asking your doctor or pharmacist whether it’s still performing as expected.
Upper‑arm vs wrist monitors: which should you choose?
Whichever type you choose, clinical validation still matters. Upper‑arm monitors are usually the simplest and most reliable option for most people, while wrist monitors can work well for some people but tend to be more sensitive to positioning and technique.

Upper-arm cuff monitors (usually best)
For most people, an upper-arm cuff monitor is usually the best option: it tends to be more reliable and is the most commonly used type in clinical settings.
UK and European organisations generally advise upper‑arm monitors where possible, because wrist monitors can be less reliable unless you follow the manufacturer’s instructions very precisely. [1, 2, 3, 4]

Wrist monitors (sometimes useful)
A wrist monitor can be useful if an upper‑arm cuff is difficult to use [2, 3, 4] — for example, if:
the upper arm is difficult to fit comfortably into a cuff
you have limited shoulder movement
an upper‑arm cuff is painful or impractical
But wrist readings are more sensitive to positioning. [3] If you use one, follow the instructions carefully — keeping the wrist steady and at heart level throughout the reading.
Bottom line: If you can use an upper‑arm cuff comfortably, choose that. If not, a clinically validated wrist model can be a good alternative — just be strict about technique.
Buying tips: how to choose a monitor that suits you
Use this checklist when you’re comparing models.
1) Clinical validation (non‑negotiable)
Only consider devices that are clinically validated. If you can’t find clear validation information, skip it.
2) Cuff fit (important for accuracy)
Before you buy, measure around your upper arm (around the bicep muscle, midway between shoulder and elbow) and check the cuff size range.
A cuff that’s too small or too large can give misleading readings and feel uncomfortable.
Tip: Some monitors come with a standard cuff; others offer small/large cuffs or a “wide range” cuff, but they will always state the cuff length in centimetres.
3) Ease of reading and ease of use
If you’re buying for yourself (or a family member), prioritise:
a clear screen with large numbers
simple buttons
straightforward instructions
4) Memory and sharing results
Consider how you’ll record readings:
Notebook log: simple and works for anyone.
Built‑in memory: useful if you don’t want to write it down.
App connection: helpful if you want automatic charts or easy sharing.
5) Features that improve accuracy
Look for features that help you take consistent readings at home, such as movement detection and averaging.
(We explain these features in more detail below.)
6) Optional: heart rhythm features
Some monitors include irregular rhythm detection and, in certain validated models, AFib detection. These can be a useful extra check — especially if you already have a history of rhythm problems, or you’ve been advised to keep an eye on your pulse.
They can also be helpful because rhythm issues are sometimes silent: you might not feel anything unusual, but a monitor may occasionally flag an irregular pattern during a reading.
They don’t diagnose a condition, but they may help you notice patterns worth discussing with a clinician. (We explain these features in more detail below.)
A practical tip: ask a clinician to check your technique (and your device)
If you can, take your monitor to a doctor or pharmacist appointment. They can help confirm:
you’re using the cuff and positioning correctly
which arm you should use (some people consistently read higher in one arm)
your home monitor’s readings are broadly in line with a clinic reading taken at the same visit
This is especially helpful when you’re new to home monitoring, changing devices, or getting unexpected readings.
Features on modern blood pressure monitors (what they mean)
You’ll see lots of features listed on product pages. Here’s what they actually do — and who they’re for.
Screen and display features
Large display: Easier to read without glasses or in low light.
Backlight: Helps if you measure in the evening or early morning.
Dual display / previous reading shown: Useful for comparing your last reading at a glance.


Cuff guidance and fit helpers
Cuff fit guide: Some monitors indicate whether the cuff is wrapped correctly.
Positioning indicators: Some show if your arm is at the right height.
These can be genuinely helpful, especially when you’re new to home monitoring.
Movement detection
Body movement detection: Alerts the user if any movement during the blood pressure reading may have compromised the measurement. This feature is to ensure more accurate and reliable blood pressure readings.
Multiple readings and averaging (a big one)
Blood pressure naturally changes from minute to minute. That’s why a single reading can sometimes be misleading.
Some monitors can:
Take 3 consecutive readings automatically
Show the average (often the most useful number for tracking)
If you want the most reliable home pattern, this feature is worth having — but it isn’t essential. You can achieve the same approach by taking 3 separate readings manually, about 1 minute apart, and recording (or averaging) them yourself. The automatic option simply makes it easier and more consistent.
Irregular rhythm detection and AFib detection
Some blood pressure monitors include a basic heart rhythm check. Because rhythm problems can be silent, these features may occasionally flag an irregular pulse pattern even if you feel fine.
Common variations include:
Irregular heartbeat detection: The monitor analyses the pulse pattern while it measures blood pressure. If it detects an irregular pattern, it may show an “irregular heartbeat” icon. This can happen for many reasons — including extra beats, movement, talking, or other rhythm changes.
In plain English: “This reading may be less reliable, and your pulse didn’t look regular.”
Atrial fibrillation (AFib) detection: Some clinically validated monitors are designed to detect pulse patterns that may be consistent with AFib.
In plain English: “This pattern could be AFib. It’s worth checking properly.”
These features do not diagnose a condition, and they do not replace a clinician’s assessment — but alerts can be a useful prompt to discuss your readings (and any symptoms) with your doctor.
Note: If an irregular pattern is detected during a reading, some monitors may warn that the result could be less accurate, or ask you to repeat the measurement. In that situation, sit quietly for a minute and repeat the reading, following the on‑screen instructions.
Integrated ECG (heart rhythm recording)
Some home devices combine blood pressure monitoring with an ECG feature to record a short rhythm trace (usually 30 seconds) of the heart’s electrical activity.
Some ECG-enabled devices can also provide an alert that the recorded trace may be consistent with AFib. This can be useful because it gives you something more concrete to share with a clinician — but it does not diagnose a condition, and any alert should be confirmed with proper medical assessment.
An ECG recording can be helpful for people who:
have been asked by a clinician to monitor symptoms (like palpitations)
want a clearer rhythm record to share with a clinician

Portability and travel-friendly designs
Tubeless / compact designs: Easier to pack and often quicker to set up.
Storage case included: Helpful if you travel or store it in a drawer.
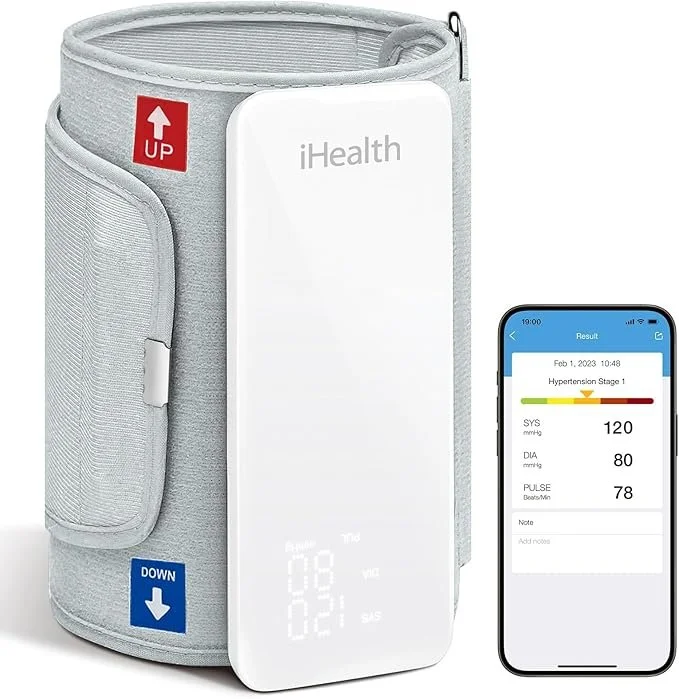

How to measure blood pressure at home
Home readings are most useful when you measure consistently.
The following steps reflect common UK/EU home-monitoring guidance. [1, 2, 3, 4]
Tip: If you can, ask your doctor or pharmacist to watch you take a reading with your home monitor. A quick check can confirm you’re using the cuff correctly, using the best arm for you, and getting results that broadly match a clinic reading.
Before you start
Avoid smoking, caffeine, alcohol, and exercise for 30 minutes beforehand.
Then sit quietly and rest for 5 minutes before measuring blood pressure.

Step-by-step
Sit with your back supported, feet flat, and legs uncrossed.
Rest your arm on a table so the cuff will be at heart level.
Using an appropriately sized cuff, place it on bare skin about 2 cm above the elbow crease, snug but not painfully tight.
Start the reading and stay still, and avoid talking during measurements.
Take 3 readings, about 1 minute apart, and use the average of the last two. Record the results in a notebook or with a connected mobile app.
Even small technique slips can affect a reading more than people realise. If you want a practical refresher on the most common problems, see our guide to “5 common mistakes when taking a home blood pressure reading.”
When you’re first checking at home
When initially checking your blood pressure at home or following an elevated reading obtained at the doctor’s surgery/health centre, a common approach is:
Measure and record your blood pressure twice daily (using an average as mentioned in step 5 above), in the morning and evening, for 7 days.
Discard the first day's measurements and calculate the average for the remaining days. This will help guide you and your doctor. [1, 2, 3]
(Always follow any plan your clinician gives you, if it differs.)
Key Takeaways: Five quick checks before you buy
Choose a clinically validated monitor.
Prefer an upper‑arm cuff if you can use one comfortably.
Get the cuff size right (measure your upper arm before you buy).
Useful extras: movement detection and averaging (automatic or manual).
Consider heart rhythm alerts: Irregular heartbeat detection or AFib detection. Rhythm problems can also be silent, so this may be a worthwhile long‑term health feature even if you feel well.
When to seek medical help
This content is for general education and does not interpret individual readings or provide medical advice.
If you’re concerned about your blood pressure or feel unwell, contact your doctor or a qualified healthcare professional.
National health organisations provide guidance on when medical attention may be needed:
NHS: High blood pressure
If you feel acutely unwell, seek urgent medical help.
To view a selection of home blood pressure monitors we consider good options (based on clinical validation and usability), click below:
Important Information:
This page is provided for general educational purposes only and does not constitute medical advice. Medical knowledge and guidance evolve over time, and information may change. Always seek advice from a qualified healthcare professional regarding personal health concerns or medical decisions.
For more details, please see our full Disclaimer.
References
National Institute for Health and Care Excellence (2019). Hypertension in adults: diagnosis and management [NG136]. London, NICE.
Stergiou GS, Palatini P, Parati G, O'Brien E, Januszewicz A, Lurbe E, Persu A, Mancia G, Kreutz R; European Society of Hypertension Council and the European Society of Hypertension Working Group on Blood Pressure Monitoring and Cardiovascular Variability. 2021 European Society of Hypertension practice guidelines for office and out-of-office blood pressure measurement. J Hypertens. 2021 Mar 11.
Parati G, Stergiou GS, Bilo G, Kollias A, Pengo M, Ochoa JE, Agarwal R, Asayama K, Asmar R, Burnier M, De La Sierra A, Giannattasio C, Gosse P, Head G, Hoshide S, Imai Y, Kario K, Li Y, Manios E, Mant J, McManus RJ, Mengden T, Mihailidou AS, Muntner P, Myers M, Niiranen T, Ntineri A, O'Brien E, Octavio JA, Ohkubo T, Omboni S, Padfield P, Palatini P, Pellegrini D, Postel-Vinay N, Ramirez AJ, Sharman JE, Shennan A, Silva E, Topouchian J, Torlasco C, Wang JG, Weber MA, Whelton PK, White WB, Mancia G; Working Group on Blood Pressure Monitoring and Cardiovascular Variability of the European Society of Hypertension. Home blood pressure monitoring: methodology, clinical relevance and practical application: a 2021 position paper by the Working Group on Blood Pressure Monitoring and Cardiovascular Variability of the European Society of Hypertension. J Hypertens. 2021 Sep 1;39(9):1742-1767.
McEvoy JW, McCarthy CP, Bruno RM, Brouwers S, Canavan MD, Ceconi C, Christodorescu RM, Daskalopoulou SS, Ferro CJ, Gerdts E, Hanssen H, Harris J, Lauder L, McManus RJ, Molloy GJ, Rahimi K, Regitz-Zagrosek V, Rossi GP, Sandset EC, Scheenaerts B, Staessen JA, Uchmanowicz I, Volterrani M, Touyz RM; ESC Scientific Document Group. 2024 ESC Guidelines for the management of elevated blood pressure and hypertension. Eur Heart J. 2024 Oct 7;45(38):3912-4018.